EMG reveals the neuromuscular strategy, not just performance outcomes
EMG measures the electrical activity of muscles, showing when muscles activate, how strongly, and how they coordinate – giving insight beyond what force, speed, or movement alone can tell you.
It exposes hidden deficits like asymmetries, compensation, and inhibition
Athletes may “look fine,” but EMG can uncover under-activation, side-to-side imbalances, or compensatory patterns – all critical for return-to-play decisions, injury risk screening, and movement quality assessment.
EMG enables more targeted, objective decision-making in rehab and performance
From biofeedback and motor control retraining to fatigue monitoring and performance profiling, EMG provides actionable data to guide programming, validate progress, and optimize outcomes in both rehab and sport settings.
Electromyography (EMG) has long been a staple in biomechanics labs, but recent advances in wearable technology and signal processing are bringing it closer to the day-to-day realities of sport, rehabilitation, and athlete monitoring. For practitioners, whether you’re a physical therapist, athletic trainer, or performance coach, EMG offers a way to bridge the gap between what you see externally and what’s happening inside the neuromuscular system.
Rather than only measuring the outcomes of movement (like speed, jump height, or ground reaction forces), EMG provides insight into the neuromuscular strategies that produce those outcomes. This is especially valuable in contexts where athletes may “look fine” from the outside, but their muscles tell a different story.
Electromyography measures the electrical activity from a muscle generated when motor units are recruited.
The motor unit is the combination of the alpha-motoneuron and the group of muscle fibers that it innervates. Each motor unit produces a distinct electrical signature, an action potential, when it fires, and the EMG signal is a summation of all of the action potentials from the recruited motor units. By placing electrodes on the surface of the skin over the target muscle area, the recorded EMG reflects the collective electrical activity that is generated by the contraction from the capture area. Surface EMG is the most common technique for this measurement in sport and rehab because it is non-invasive and can record activity during dynamic movements.
Think of force outcomes as the speedometer on a car. It can tell you how fast the car goes. EMG is your engine investigative tool; it shows you which cylinders are firing, in what sequence, and whether the engine is working efficiently. The car might be going really fast, but all the engine warning lights could be on.
EMG reflects the neural drive to the muscle, not the force produced. The level of muscle activation can be mediated by two factors commonly. Either a particular motor unit can fire more frequently, or additional motor units can be recruited.
However, more EMG does not always scale linearly to more force due to variances in muscle length, joint position, mechanical properties, muscle architecture, and other physiological and anatomical factors.
During muscle contractions and dynamic movements, EMG is typically normalized to a maximum voluntary contraction (MVC) and reported as a relative value to reduce the influence of intrinsic factors on the EMG signal. The mechanical output of torque or force is also important to be able to capture when characterizing the relationship with EMG activity of a single muscle or a group of muscles.
When interpreting EMG in the context of force outcomes, it is also important to consider the scenario in which the data is being collected and the question being asked of the relationship.
| Scenario | EMG | Force | Interpretation |
|---|---|---|---|
| Increasing effort in good mechanics | Increase | Increase | More neural drive ≈ more force with strong form and technique. |
| Late-rep fatigue in heavy work | Increase | Decrease | High neural drive struggling to compensate to meet the mechanical demands of the task. |
| Poor technique / early rehab | Increase | Stable / Decrease | Inefficient recruitment compared to mechanical output. |
| Improved skill after training | Decrease | Stable / Increase | Same or stronger with less neural cost. More efficient task execution. |
For many years, EMG was confined to research labs because of bulky equipment and complex analysis requirements. But with modern wireless systems and streamlined software, its applications are expanding. Example key areas include:
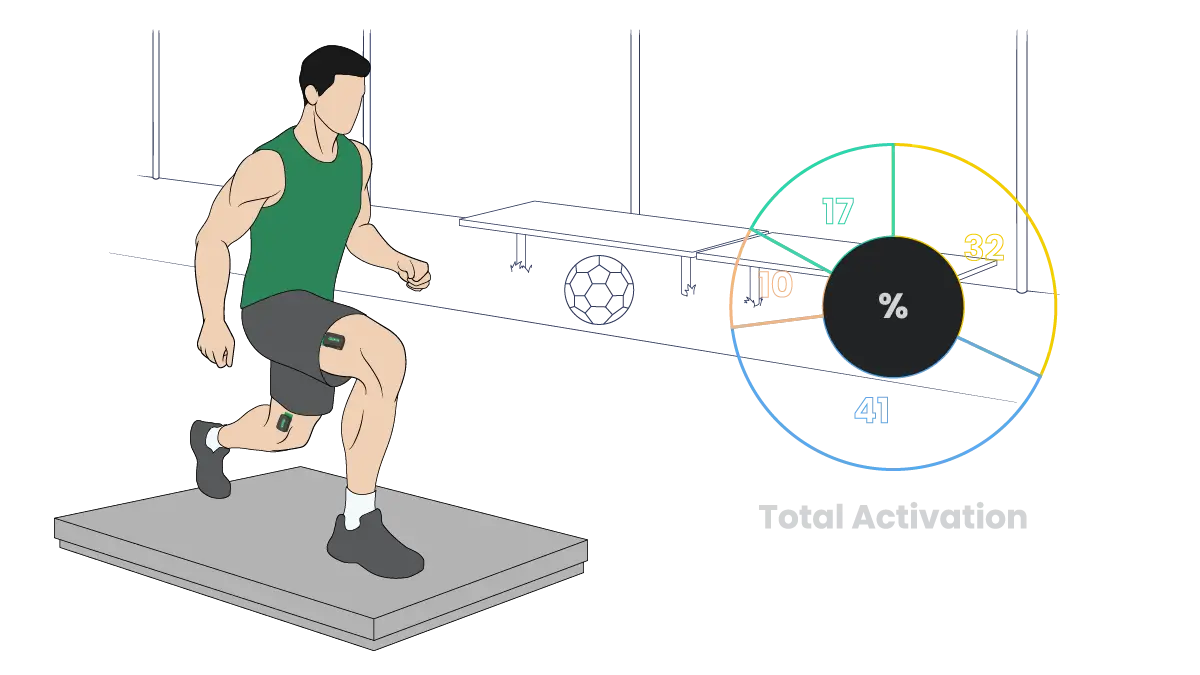
After ACL reconstruction, athletes often demonstrate arthrogenic muscle inhibition in the quadriceps. Even if strength tests look solid, EMG can show persistent under-activation during functional tasks. This provides objective evidence for progressing rehab or delaying return.

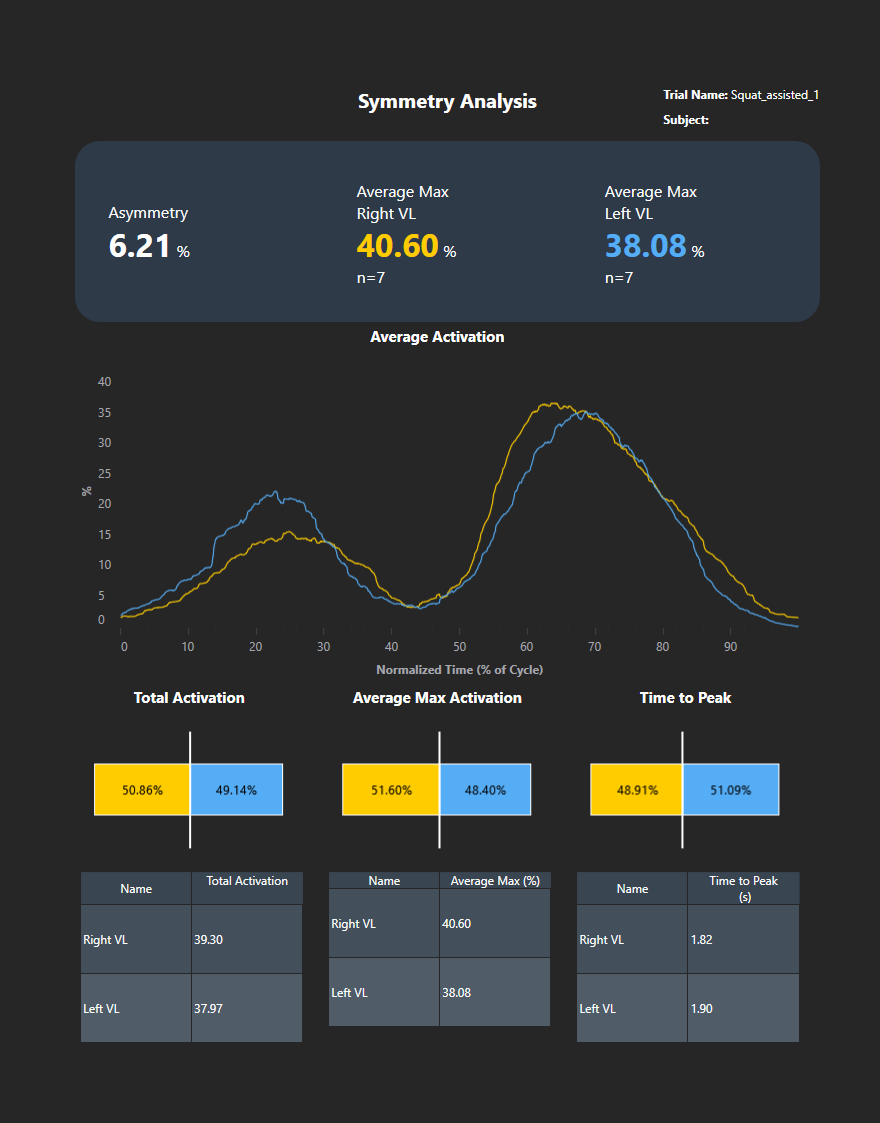
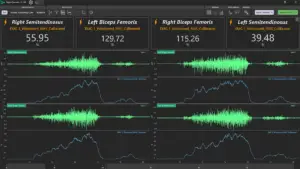
During squats, athletes may offload to the opposite leg due to injury compensations or improper technique. EMG can reveal left–right differences in quadriceps activation, helping identify asymmetries and promote more balanced muscle recruitment.
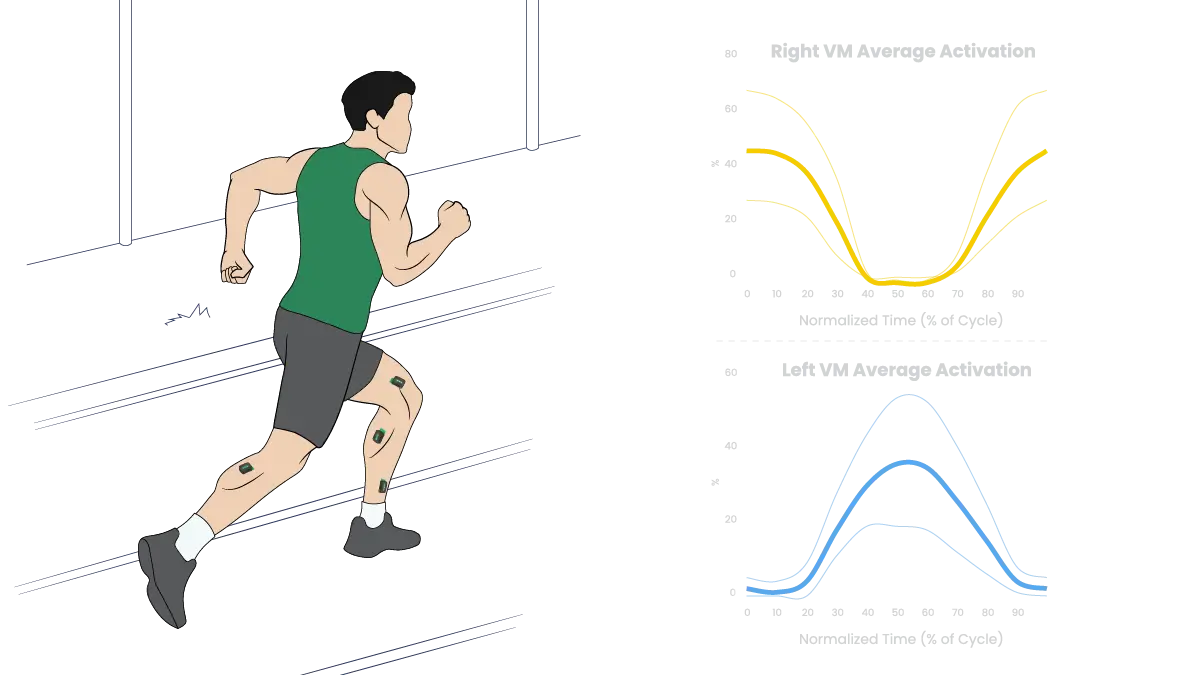
During sprint accelerations, EMG can reveal whether an athlete relies excessively on hip extensors while under-recruiting quadriceps. This information can inform strength programming or technical coaching.
In-season, EMG can be used to monitor neuromuscular fatigue, identifying shifts in activation timing and amplitude profiles or decreases in median frequency that indicate muscle fatigue before it shows up in performance decline.
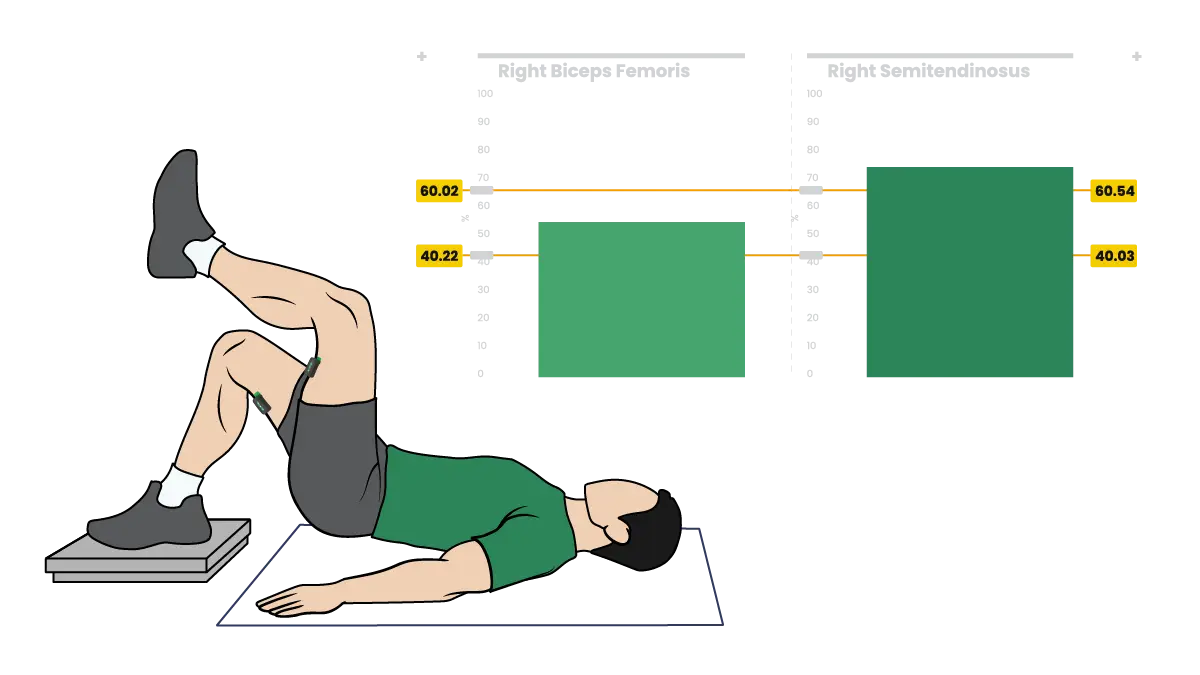
Athletes returning from lower limb injury can use EMG-driven biofeedback to identify and correct hamstring compensation patterns, helping restore balanced activation and reduce asymmetries during rehab and return-to-play progressions.
Depending on the rehabilitation or performance question, EMG can be interrogated in several ways:
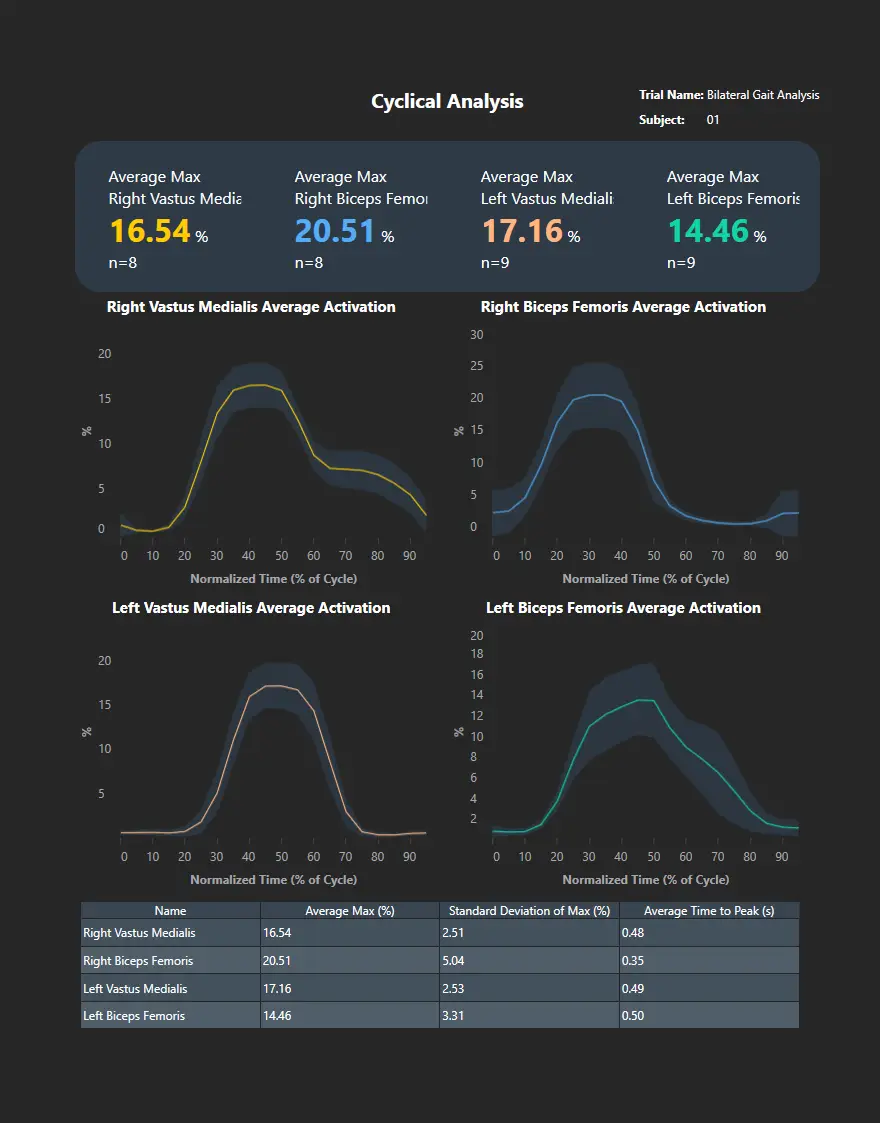
When muscles activate relative to events like heel strike, take-off, or pedal cycles. Useful for gait retraining or technical analysis in sport for repetitive tasks.
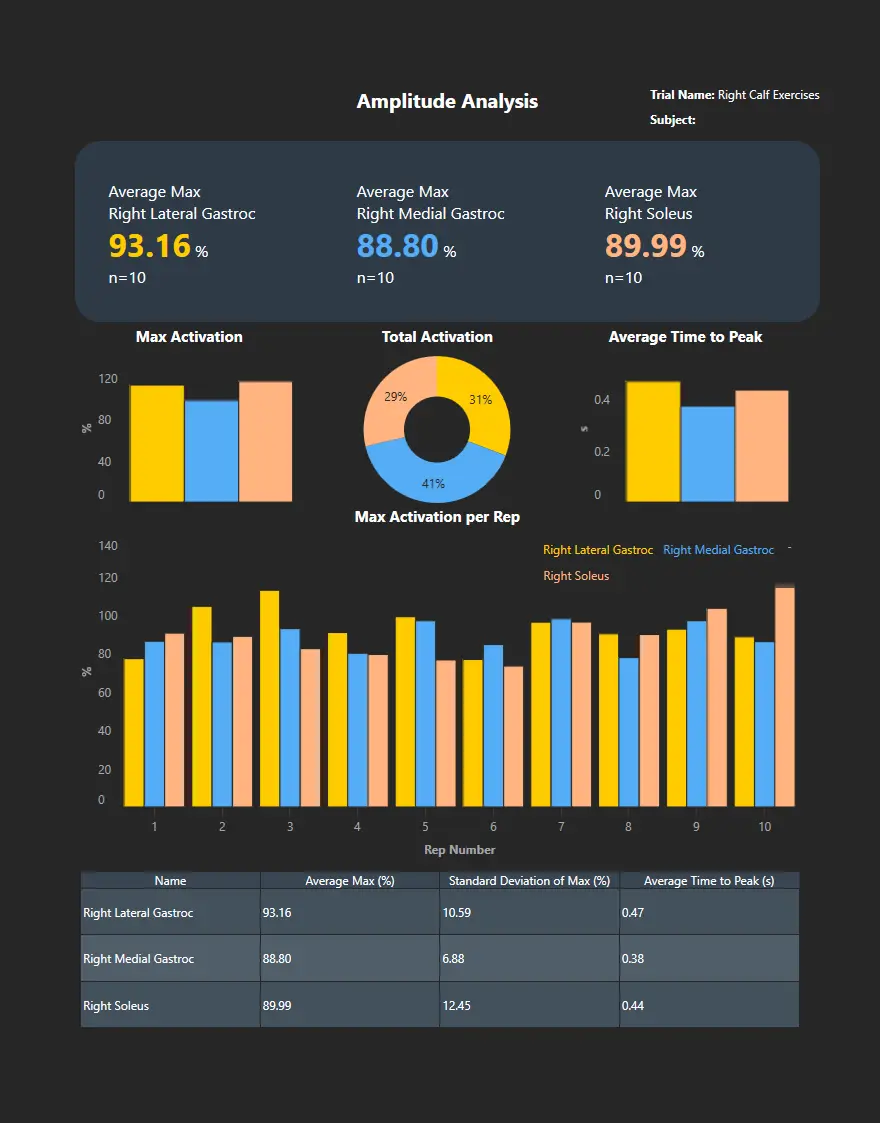
The magnitude of activity is often expressed relative to a maximum voluntary contraction (MVC). This analysis provides insight into recruitment intensity and how this varies over time and across exercises.
Comparing left vs. right sides, or muscles within a muscle group, for amplitude, timing, or patterns. This analysis is essential for return-to-play and injury prevention monitoring.
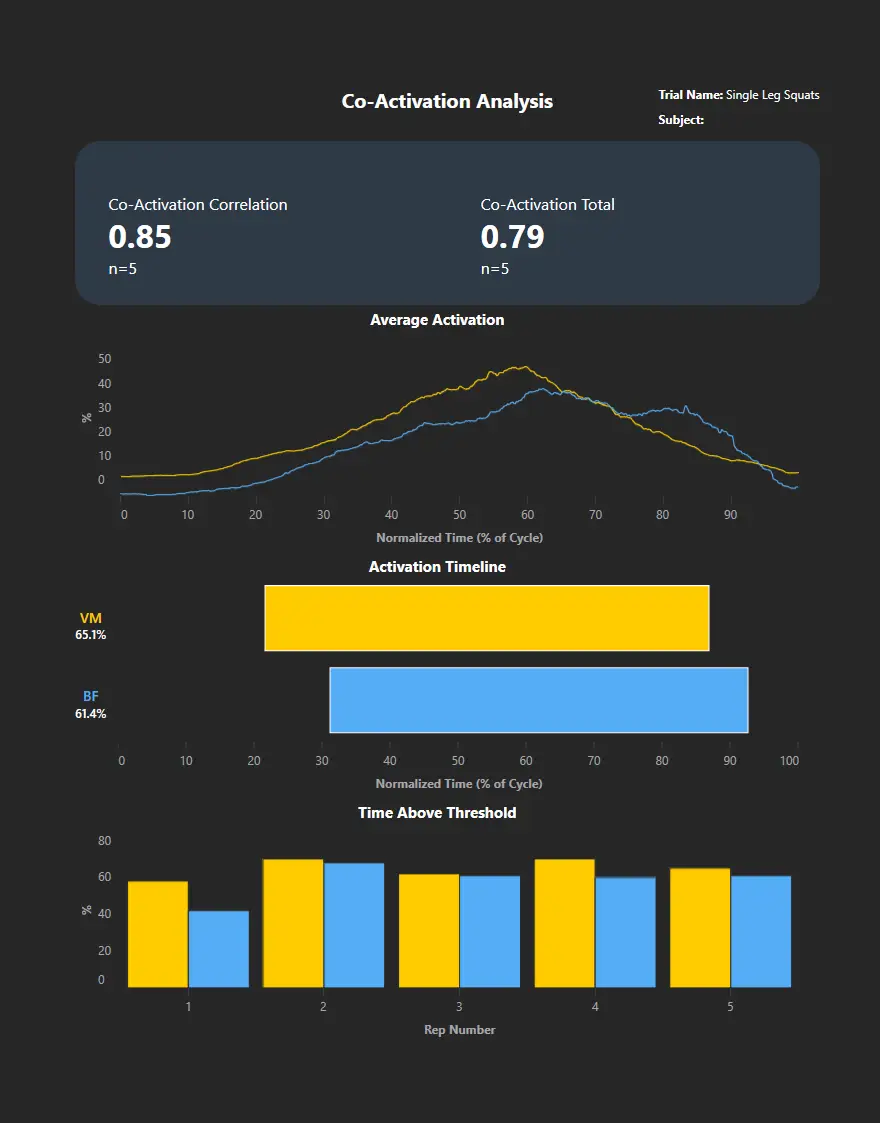
How multiple muscles coordinate agonists, antagonists, and stabilizers. High co-activation may stabilize joints but also increase metabolic cost. High co-activation can also be a sign of impairment with the muscle being unable to “turn-off”.
Examines the frequency content of the signal. A downward shift in frequency can be a marker of neuromuscular fatigue when performed under isometric conditions.
EMG can be powerful, but like any tool, its value depends on setup and interpretation. Some key points to keep in mind:

Placement must be consistent and anatomically precise. Guidelines like SENIAM help standardize this, but practitioner training is key.
Shaving, cleaning, and prepping the skin reduces impedance and improves signal quality. Poor preparation can lead to noisy and unreliable data.
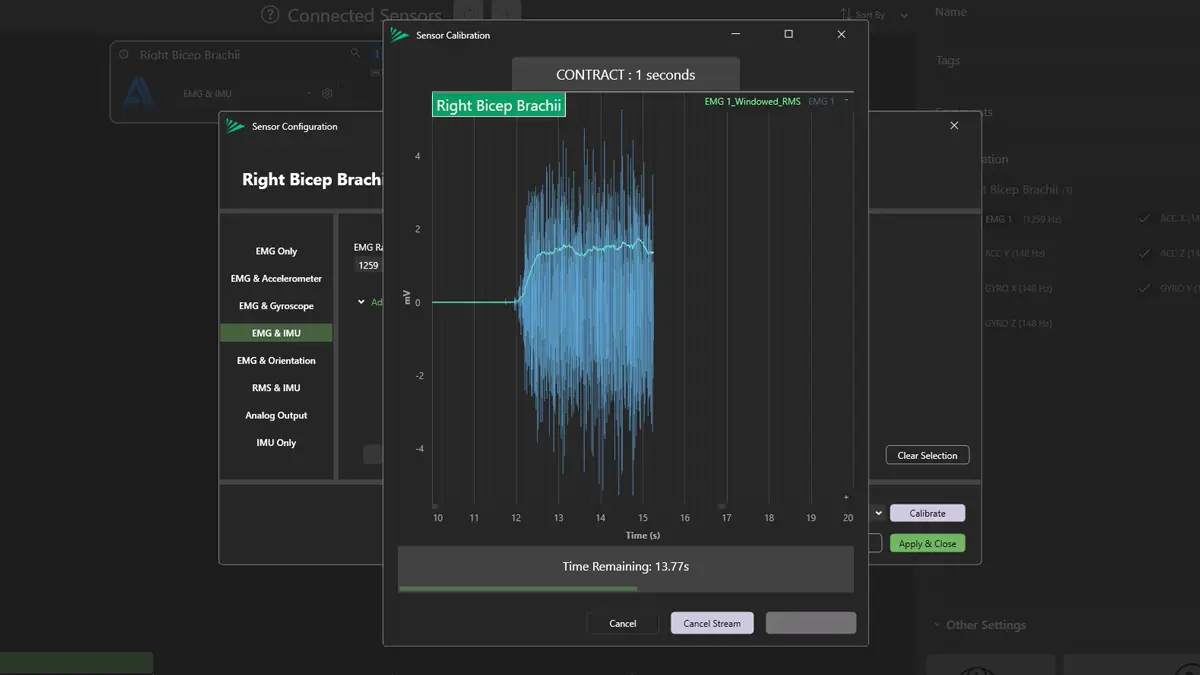
Comparing EMG amplitude across sessions or athletes requires a reference. This is often a maximal voluntary contraction, but standardized submaximal tasks can also work depending on context.
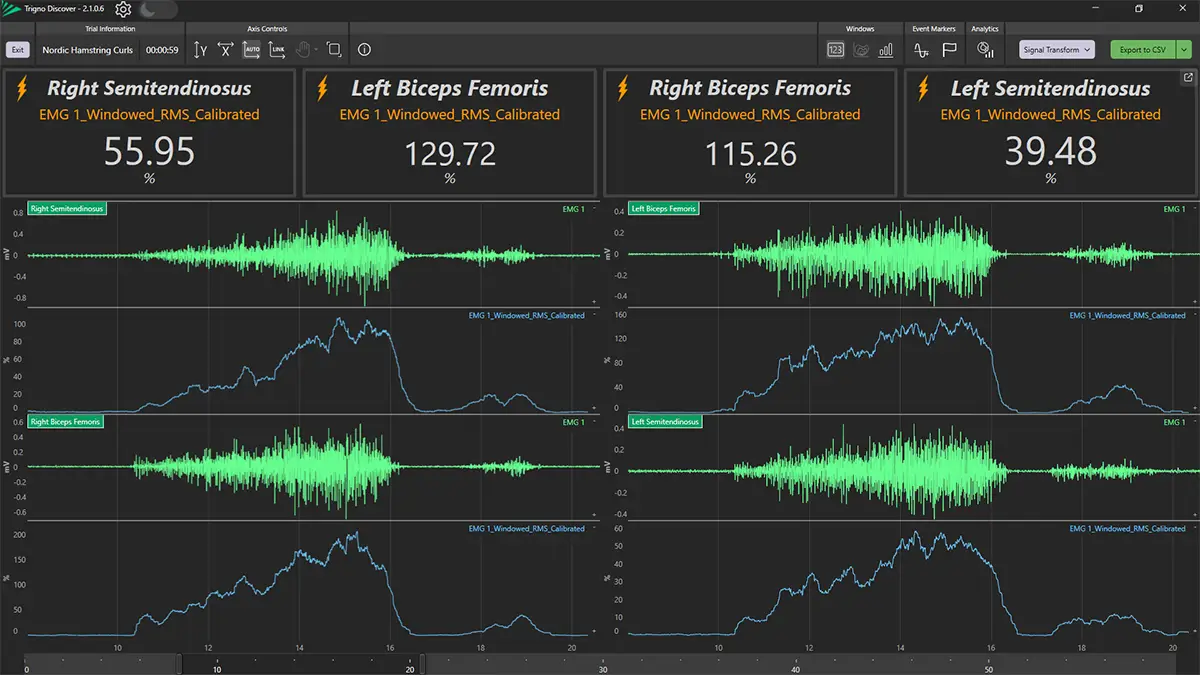
EMG does not equal muscle force. Signal amplitude reflects neural drive, which interacts with factors like muscle length, fatigue, and electrode position. Always interpret within context.
EMG is most valuable when combined with kinematics (motion capture), kinetics (force plates), or other wearable sensor data. Alone, it gives partial insight; together, it builds a complete picture.


Shaving, cleaning, and prepping the skin reduces impedance and improves signal quality. Poor preparation can lead to noisy and unreliable data.
1 of 5 2 Electrode Placement
Placement must be consistent and anatomically precise. Guidelines like SENIAM help standardize this, but practitioner training is key.
2 of 5 3 Normalization Comparing EMG amplitude across sessions or athletes requires a reference. This is often a maximal voluntary contraction, but standardized submaximal tasks can also work depending on context.
Comparing EMG amplitude across sessions or athletes requires a reference. This is often a maximal voluntary contraction, but standardized submaximal tasks can also work depending on context.
EMG does not equal muscle force. Signal amplitude reflects neural drive, which interacts with factors like muscle length, fatigue, and electrode position. Always interpret within context.
4 of 5 5 Data IntegrationEMG is most valuable when combined with kinematics (motion capture), kinetics (force plates), or other wearable sensor data. Alone, it gives partial insight; together, it builds a complete picture.
5 of 5For physical therapists, EMG can confirm whether target muscles are truly “back online” before patients progress to higher-level activities. For athletic trainers, it highlights compensations invisible to the naked eye. And for performance coaches, it offers an extra dimension of insight into how force is actually being produced, helping refine training strategies and prevent overload.
The technology is no longer confined to research labs. With modern portable systems, EMG can become part of your applied toolkit. Used thoughtfully, it elevates clinical reasoning, enriches athlete profiling, and ultimately supports better outcomes on the field, in the clinic, and in the weight room.
For more information, please reach out to contact@delsys.com.